Xylazine: Still a Threat
Author: Dr. JP Canner, Ph.D., NRCC, MT(AAB)
Xylazine: Still a Threat
In April 2023, Xylazine was designated as an emerging threat to the United States after a series of reports from the FDA (Food and Drug Administration) and DEA (Drug Enforcement Administration). (1) While the dangers of Xylazine have been documented, the prevalence of Xylazine still persists. This article will describe Xylazine and the recent history of human misuse of this sedative. We will provide evidence on why Xylazine persists in the illicit drug supply and lastly detail trend data observed within our specimen data highlighting the regional patterns of use.
What is Xylazine?
Xylazine is an alpha-2 agonist that inhibits the release of presynaptic norepinephrine. This mechanism is responsible for the sedative effects of Xylazine as well as hypotension. Clinical use of Xylazine in humans was abandoned due to side effects but was approved for veterinary use by the FDA in 1972. (2) Xylazine is routinely used in large animal care as an analgesic/sedative and oftentimes as a commixture with Ketamine during surgical procedures. (3)
History of Human Abuse
Most studies cite the first prolonged abuse of Xylazine to arise in Puerto Rico, with Xylazine being cut into heroin supplies, and a common additive to opioid-stimulate mixtures.(4) The stability of Xylazine in this supply could be attributed to perception that Xylazine prolongs the sedative effects of opioids.(2) However, surveys typically find that most persons who inject drugs (PWID) view Xylazine as an unwanted adulterant.(4) The current rise in Xylazine abuse in the continental US is believed to have originated in the Philadelphia street opioid supply, sometimes sought out to increase the duration of the fentanyl high.(5) The addition of Xylazine to the illicit Fentanyl supply spread throughout the Northeast and traveled westward.(6) Between 2018 to 2021, there was a 1238% increase in drug-poisoning deaths in the US involving Xylazine.(2)
Dangers of Xylazine
The dangers of Xylazine illicit drug use include respiratory depression that can result in cessation of breathing. Unlike opioids, there is no antidote to reverse the action of Xylazine, such as administrating Naloxone for patients on Fentanyl. A further complication is ulcerative wounds that develop in individuals using Xylazine. A common belief is that the wounds occur at the inject site, but they result from Xylazine’s vasoconstrictive properties causing reduced blood flow to the skin.(4) Therefore, these wounds are observed in non-injection sites and are typically the sign of Xylazine use.(2) Lastly, there have been a few cases of withdrawal symptoms in individuals with chronic use of Xylazine, but data is limited.(4)
Current Data
Since being declared an emerging threat, the supply of Xylazine for veterinary use has been more closely monitored and efforts to reduce the influx of foreign products have occurred. (3) However, these have not been able to completely remove Xylazine from the illicit supply chain. Our internal data from clinical toxicology testing shows that Xylazine is entrenched in the Northern Kentucky region (Figure 1). Given the history of opioid misuse, it is no surprise that this region has seen Xylazine introduced into the illicit Fentanyl supply. The percentage of Fentanyl positive specimens with Xylazine in Northern Kentucky is 23% higher than the Commonwealth of Kentucky. Interestingly, the rate of Xylazine use has stayed consistent over the past 4 months, compared to the rise observed in the US over the past 5 years. Across our US data set, we see 49% of Fentanyl positives specimens have detectable levels of Xylazine.
Next Steps
The data suggests a leveling of Xylazine use, but it has become entrenched in regional illicit Fentanyl supply. As described earlier, the perceived benefit of a prolonged “legs” means this adulterant has staying power, despite the gruesome skin wounds. Future work is needed to understand the best treatment options for these PWID with chronic Xylazine exposure, and potential antagonist to counteract acute toxicity.
Gravity Diagnostics’ Role
Gravity Diagnostics is committed to the efforts of curbing substance use disorders, particularly in our Northern Kentucky region. Understanding what substances are in the illicit supply is critical to inform the community of best treatment options, and the data generated by Gravity Diagnostics is key to that understanding. We built out several reporting options to share information of specific patient populations, regional trends, and co-detection rates of illicit substances to ensure clinicians are abreast of changing substance use preferences.
If you or someone you know is struggling with substance abuse, reach out to the Substance Abuse and Mental Health Services Administration National Helpline at 1-800-662-4357.
References:
https://www.whitehouse.gov/ondcp/briefing-room/2023/04/12/biden-harris-administration-designates-fentanyl-combined-with-xylazine-as-an-emerging-threat-to-the-united-states/
Gupta R, Holtgrave DR, Ashburn MA. Xylazine - Medical and Public Health Imperatives. N Engl J Med. 2023 Jun 15;388(24):2209-2212. doi: 10.1056/NEJMp2303120. Epub 2023 Apr 26. PMID: 37099338.
https://www.fda.gov/animal-veterinary/news-events/what-were-doing-stop-illicit-xylazine-getting-us
Papudesi BN, Malayala SV, Regina AC. Xylazine Toxicity. [Updated 2023 Jul 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK594271/
Montero, F., Bourgois, P. and Friedman, J., 2022. Potency-Enhancing Synthetics in the Drug Overdose Epidemic: Xylazine (“Tranq”), Fentanyl, Methamphetamine, and the Displacement of Heroin in Philadelphia and Tijuana. Journal of Illicit Economies and Development, 4(2), p.204–222.DOI: https://doi.org/10.31389/jied.122https://jied.lse.ac.uk/articles/10.31389/jied.122
DEA Joint Intelligence Report. The Growing Threat of Xylazine and its Mixture with Illicit Drugs. October 2022. DEA-DCI-DIR-001-23. https://www.dea.gov/alert/dea-reports-widespread-threat-fentanyl-mixed-xylazine
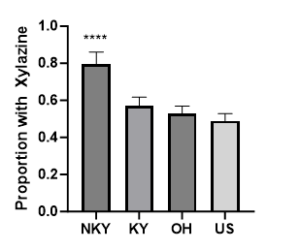
Figure 1: Proportion of Fentanyl containing urine specimens with detectable Xylazine. Weekly analysis of urine toxicology data from October 9th, 2023, to February 4th, 2024, shows a higher rate of detection of Xylazine in specimens from Northern Kentucky (NKY), when compared to Kentucky (KY), Ohio (OH), or all specimens (US). **** p < 0.00001.
To learn more about our toxicology testing services, click here
